DOD warfighter brain health draft plan has six priorities
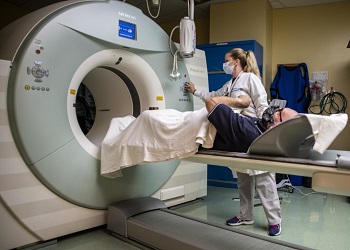
 Lorie Falaminiano, an MRI technologist at Naval Medical Center San Diego, conducts a scan of a patient's brain Aug. 3. Brain scans that occur on a more frequent basis during a warfighter’s military career and beyond are one of the six concerns and priorities outlined by operational service members. (Photo by Navy Mass Communication Specialist Seaman Luke Cunningham.)
Lorie Falaminiano, an MRI technologist at Naval Medical Center San Diego, conducts a scan of a patient's brain Aug. 3. Brain scans that occur on a more frequent basis during a warfighter’s military career and beyond are one of the six concerns and priorities outlined by operational service members. (Photo by Navy Mass Communication Specialist Seaman Luke Cunningham.)
Documenting how warfighters score on cognitive testing – from the beginning of their careers until after they leave military service – is one of six major concerns and priorities of service members being addressed in a plan for brain health that is in final draft form.
This change to looking at brain exposures and traumatic brain injury (TBI) across the warfighter’s entire career represents a “paradigm shift” in the Department of Defense’s approach, TBI specialist Kathy Lee told the Society of Trauma Nurses annual conference, held virtually March 26.
Lee, senior health policy analyst for DOD’s Health Affairs, discussed the comprehensive strategy and plan for warfighter brain health (WBH), which addresses brain health, brain exposures, including blast exposures, TBI, and long-term and late effects of exposures and/or TBI.
General physical and brain health assessments, scans, or tests “that occur on a more frequent basis over time across their military careers and beyond if deficits are identified” is one of the six concerns and priorities outlined by operational service members, according to Lee.
Dissemination of information on which “brain exposures are most damaging” and “outright disclosure if they are at increased risk of exposure or injury while performing a specific training activity” such as breaching walls or experiencing blast overpressure is another priority and concern for transparency.
There are “multiple, deleterious effects of exposures before traumatic brain injury actually occurs” as well as TBI itself, Lee said. Known and emerging brain exposures are: blast overpressure; blunt force/impact; projectiles; directed energy (high-powered microwave); chemical-biological toxins; and other environmental hazards, she explained.
 Michelle Pribble, Naval Medical Center San Diego's lead nuclear medicine technologist, prepares a patient for a positron emission tomography (PET) scan in the hospital's Nuclear Medicine Department Oct. 6. A PET scan is used for revealing or evaluating conditions including brain disorders. (Photo by Navy Mass Communication Specialist Seaman Luke Cunningham.)
Michelle Pribble, Naval Medical Center San Diego's lead nuclear medicine technologist, prepares a patient for a positron emission tomography (PET) scan in the hospital's Nuclear Medicine Department Oct. 6. A PET scan is used for revealing or evaluating conditions including brain disorders. (Photo by Navy Mass Communication Specialist Seaman Luke Cunningham.)
“Upwards of 86 percent of traumatic brain injuries are classified as mild” and are known as concussions, she said. “We can see 14,000 to 17,000 patient visits per month for TBI in the military health system, which is why we need standardized tools and research” to identify, control, and mitigate these brain exposures and TBIs.
The other four concerns expressed by service members are:
- “Perceived disconnect” between operational efforts in preparation and training for combat and “medical communities translating brain health information to the service member in time to help them,” Lee said.
- “Warrior mindset” that can discredit a service member’s own struggles or concerns “because they have a desire to complete their mission despite brain exposures, injury or illness” and “because they often compare themselves to other service members who may be in worse condition,” she said.
- “Multiple concerns” over the newer emphasis on blast overpressure exposures and brain health and how safety and training changes may dilute training opportunities, deployment readiness and force lethality.
- “Clinical tools, protocols, and research solutions” if the service member has been in the military longer and “may be noticing changes in functional abilities.”
All service members are required to take the Automated Neuropsychological Assessment Metrics test (ANAM) prior to deployment. The test has been in use since 2008 and has 10 domains to set up a baseline of cognition, which is one marker of brain health, Lee said.
“In fiscal 2019, we completed more than 220,000 of these assessments,” she said. “The WBH proposed plan will expand that requirement to include conducting the ANAM on all service members so that we can monitor and optimize cognitive performance and maximize combat effectiveness,” she said.
The WBH draft plan has 18 objectives and 53 associated activities along five “lines of effort” for “the deliberate, prioritized, and rapid development of end-to-end solutions,” Lee explained.
The five lines of effort are:
- Optimize cognitive and physical performance
- Identify, monitor, and mitigate brain exposures
- Prevent, recognize, and minimize the effect of TBI
- Reduce or eliminate long-term/late effects
- Advance warfighter brain health science
The research and science objectives of the DOD plan are to “align brain health research and acquisition to current and emerging threats and operational requirements;” “maximize WBH research opportunities for partnerships with other government agencies, industry, and academia;” “enable researchers to have access to valid data regarding brain exposures and injuries and related brain health effects;” and “translate research findings into knowledge and materiel products, practice, and policies to maintain and optimize WBH,” Lee said.
Some of the research involves evaluating the late effects following blast and multiple TBIs by examining the brains of more than 200 service members from a repository at the Uniformed Services University of Health Sciences in Bethesda, Maryland, Lee noted.
Research includes examinations of clinical diagnoses, blood-based biomarkers, genetics, diagnostic imaging, and outcomes after treatment. A new rapid blood biomarker for TBI was cleared recently by the Food and Drug Administration for use in austere environments, adding to the armamentarium of biomarker tests.
The WBH plan is based on an Oct. 1, 2018, directive from DOD stating there should be a “single approach to brain health” in warfighters of all services that goes from brain exposure to TBI.
“Prior to this directive, there have been successful but disparate efforts,” Lee said.
The plan has been created through 18 months of field work and working groups, she noted. It is anticipated that the plan will be approved prior to the end of the fiscal year.
Her presentation was the first time the Society of Trauma Nurses had heard about the DOD plan, said society President Maria McMahon. It was noteworthy for practitioners because the DOD Warfighter Brain Health construct lends itself to nurse practitioner engagement in clinical practice, patient education, policy development, and emerging research.
Lee previously presented the data at December’s annual meeting of AMSUS, The Society of Federal Health Professionals, and the draft plan was part of a November 2020 themed issue of the Journal of the American Association of Nurse Practitioners.