METC NDT trainees learn about brain disorders & care
 METC NDT trainees learn about brain disorders & care
METC NDT trainees learn about brain disorders & care
Neurodiagnostic Week, April 18-24, is an annual campaign that serves to bring attention to and acknowledge the efforts of neurodiagnostic professionals around the world. This year in particular has been particularly challenging with the Coronavirus pandemic, as neurodiagnostic technologists (NDT) face additional challenges while remaining committed to providing a high-level of patient care.
NDTs, including those in the military, perform many tests that diagnose problems with the brain and nervous system, as well as sleep disorders. They use state-of-the-art digital equipment to record electrical patterns throughout the brain and nervous system, which result in valuable data that the doctor needs to diagnose and treat their patients. The data gathered from these tests can help diagnose conditions like epilepsy, other seizure disorders, strokes, degenerative brain disease, and traumatic brain injuries, among others. Military NDTs usually work in hospitals and clinics.
Military NDT training is conducted at the Medical Education and Training Campus (METC) on Joint Base San Antonio-Fort Sam Houston, Texas. Students in the METC NDT program arrive with a medical background, either as a Navy hospital corpsman or Air Force medical technician.
Air Force Tech. Sgt. Stephanie Shishido, service lead and instructor for the METC NDT program, is one of only 48 neuro techs in the entire military.
"The NDT career field is amazing to me," she stated. "We have the autonomy to work independently from a neurologist, and our studies can directly dictate the course of treatment and/or diagnosis."
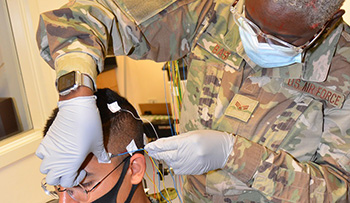 Air Force Senior Airman Jamila Basit, a student in the Neurodiagnostic Technician program at the Medical Education and Training Campus, practices the electrode application method required for performance of the Electroencephalogram (EEG) on fellow student, Navy Seaman Marcus Falcon (Photo by: Lisa Braun, Medical Education and Training Campus).
Air Force Senior Airman Jamila Basit, a student in the Neurodiagnostic Technician program at the Medical Education and Training Campus, practices the electrode application method required for performance of the Electroencephalogram (EEG) on fellow student, Navy Seaman Marcus Falcon (Photo by: Lisa Braun, Medical Education and Training Campus).
The program is split into two phases. Phase 1 takes place inside the METC medical instructional facility classroom and simulated laboratory where students learn how to use specialized equipment and perform a variety of procedures to diagnose numerous disorders and diseases. One of the most common tests that NDT students learn is the electroencephalograms (EEG), used to assess brain activity. Students also learn how to perform other tests that detect and record magnetic fields in the brain, track brain and nerve function during surgery, and diagnose sleep disorders.
In phase 2, students transition to both civilian and military medical treatment facility (MTF) in the local San Antonio area, where they conduct the clinical portion of the training that includes hands-on patient care. This portion of the course provides students practical experience with hands-on patient care, enhancing their medical knowledge and proficiency. This training prepares students to exercise judgment and accept responsibility in performing diagnostic procedures while performing patient care.
Additionally, METC NDT students are afforded an opportunity to challenge a national certification exam and graduate as registered EEG technologists.
Air Force Senior Airman Christine Smith, a student in the program, was first introduced to NDT when she attended a career fair while enrolled in the METC Aerospace Medical Service Apprentice program.
"I enjoy being able to specialize and be able to learn about various brain disorders and how to diagnose them," Smith said. "I have always been fascinated with the human mind and am now very excited to learn all about the human brain!"