Abstract
This report provides an update through June 2021 of the results of routine screening for antibodies to the human immunodeficiency virus (HIV) among members of the active and reserve components of the U.S. Armed Forces and through Dec. 2020 among civilian applicants for military service. During the surveillance period, seroprevalences among applicants for service were highest in 2019 (0.36 per 1,000 tested) and then decreased in 2020 (0.32 per 1,000 tested). Full-year seroprevalence peaked in 2019 for active component service members of the Army, in 2017 for the Navy, 2018 for the Marine Corps, and 2016 for the Air Force. Among reserve and National Guard members, seroprevalence peaked in 2019 for the Air Force National Guard, 2016 for the Air Force reserve, in 2017 for the Marine Corps reserve, 2018 for the Navy reserve, and in 2016 for the Army National Guard and reserve. Overall (Jan. 2016–June 2021) HIV antibody seroprevalences were highest among Army reservists, Army National Guard members, and Navy reservists and lowest among Air National Guard members, Marine Corps active component members, and Air Force active component members. Across active and reserve components of all services, HIV antibody seroprevalences continued to be higher among men than women.
What Are the New Findings?
From Jan. 2016 through Dec. 2020, the rates of HIV test positivity among civilian applicants for military service were stable at 0.33 per 1,000 tested. Among uniformed personnel (active component, Guard, and reserve), rates between Jan. 2016 and June 2021 remained relatively stable. Rates among female applicants and female service members have remained very low compared to those of male applicants and service members.
What Is the Impact on Readiness and Force Health Protection?
The routine screening for antibodies to HIV for over 30 years has enabled the U.S. military to provide adequate and timely medical care to infected service members, counseling to prevent unwitting transmission, and protection of the battlefield blood supply.
Background
Since acquired immune deficiency syndrome (AIDS) was first recognized as a distinct clinical entity in 1981,1its spread has had major impacts on the health of populations and on health care systems worldwide. Human immunodeficiency virus type 1 (HIV-1) was identified as the cause of AIDS in 1983. For more than 30 years, the U.S. military has conducted routine screening for antibodies to HIV-1 to enable adequate and timely medical evaluations, treatment, and counseling; to prevent unwitting transmission; and to protect the battlefield blood supply.2,3
As part of the U.S. military's total-force HIV screening program, civilian applicants for military service are screened for antibodies to HIV during pre-accession medical examinations. Infection with HIV is medically disqualifying for entry into U.S. military service.4 Since 1986, all members of the active and reserve components of the U.S. Armed Forces have been periodically screened to detect newly acquired HIV infections. In 2004, the Department of Defense (DOD) set a standard testing interval of 2 years for all service members.5,6 In addition, all military personnel are supposed to be screened for HIV infection before deployment, upon return from deployment, and after having received a diagnosis of various other conditions, such as a sexually transmitted infection.6 Routine HIV screenings are usually performed during the periodic health assessment, an annual evaluation of a service member's medical readiness status. Service members who are infected with HIV receive clinical assessments, treatments, and counseling; they may remain in service as long as they are able to fully perform their military duties.2,3 HIV positive service members are eligible for certain non-combat or non-contingency deployments and, as such, must meet the DOD's retention policy for non-deployable service members. The latest policy on retention determinations for non-deployable service members was implemented in Oct. 2018 and requires service members who are in a non-deployable status for more than 12 consecutive months to be evaluated for a retention determination by their respective military departments or, as appropriate, be referred into the Disability Evaluation System, or processed for administrative separation from the military.7
Before 2009, all of the aforementioned screening programs used laboratory techniques that detected only HIV-1–type infections. Starting in 2009, all programs adopted methods that allowed the detection of antibodies to both major HIV types (i.e., HIV-1 and HIV-2). Although HIV-2 infection is rare in the U.S. and no instances of HIV-2 infection have thus far been detected in civilian applicants or service members since 2009, HIV-2 is much more prevalent in other parts of the world where service members may be required to serve. To provide for the change in laboratory methods in the past and for the prospect of future detections of HIV-2 infection in the services' screening programs, this report will hereafter refer to the target of the screening programs as simply "HIV" without specifying the types.
This report summarizes numbers, seroprevalences, and trends of newly identified HIV antibody positivity among civilian applicants for military service and members of the active and reserve components of the U.S. Armed Forces from 1 Jan. 2016 through 30 June 2021. Summaries of the results of routine screening for antibodies to HIV among civilian applicants and active and reserve component members of the U.S. military since 1990 are available at www.health.mil/MSMRArchives.
Methods
The surveillance period was Jan. 1, 2016 through June 30, 2021 for service members, and Jan. 1, 2016 through Dec. 31, 2020 for civilian applicants for U.S. military service. The surveillance population included all civilian applicants for U.S. military service and all individuals who were screened for antibodies to HIV while serving in the active or reserve component of the Army, Navy, Air Force, or Marine Corps during the surveillance period.
All individuals who were tested and all first-time detections of antibodies to HIV through U.S. military medical testing programs were ascertained by matching specimen numbers and serologic test results to the personal identifiers of providers of the specimens. All results were accessed from records routinely maintained in the Defense Medical Surveillance System (DMSS). The surveillance period was truncated to 31 Dec. 2020 for civilian applicants for U.S. military service because, at the time of analysis, the U.S. Military Entrance Processing Command (MEPCOM) had stopped providing data into the DMSS.
An incident case of HIV antibody seropositivity was defined as 2 positive results from serologic testing of 2 different specimens from the same individual or 1 positive result from serologic testing of the most recent specimen provided by an individual.
Annual prevalences of HIV seropositivity among civilian applicants for service were calculated by dividing the number of applicants identified as HIV-antibody seropositive during each calendar year by the number of applicants tested during the corresponding year. For annual summaries of routine screening among U.S. service members, denominators were the numbers of individuals in each component of each service branch who were tested at least once during the relevant calendar year.
Results
Civilian applicants
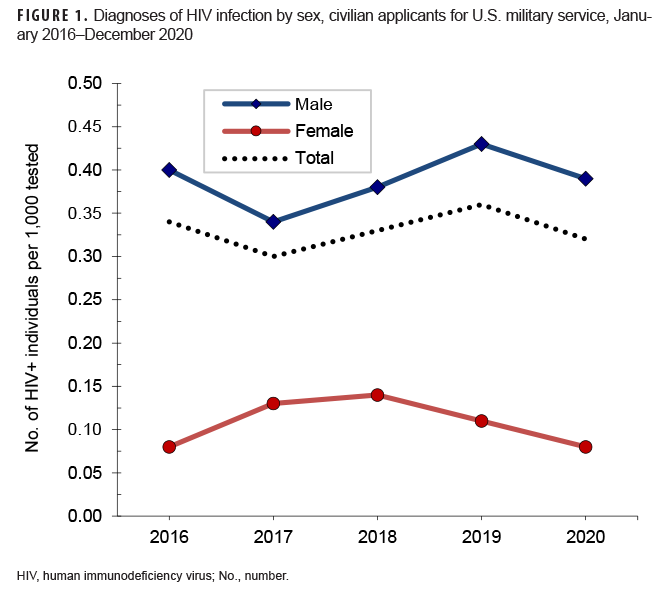
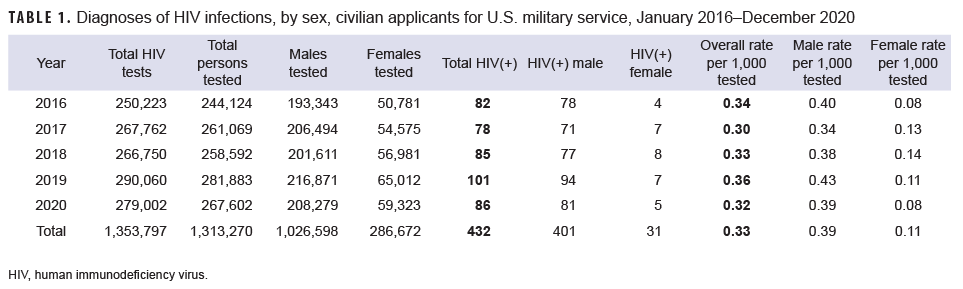
In 2020, a total of 267,602 civilian applicants for U.S. military service were tested for antibodies to HIV, and 86 applicants were identified as HIV antibody positive (seroprevalence: 0.32 per 1,000 applicants tested) (Table 1). During the surveillance period, seroprevalences among applicants for service were highest in 2019 (0.36 per 1,000 tested) and then decreased to 0.32 per 1,000 tested in 2020 (Table 1, Figure 1).
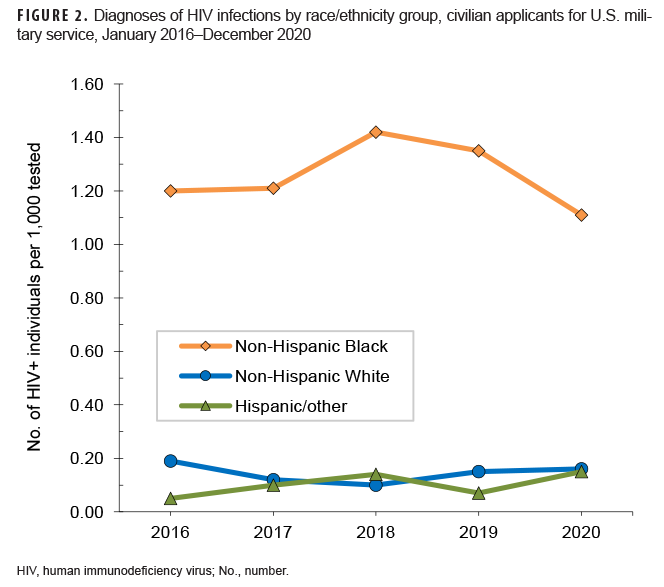
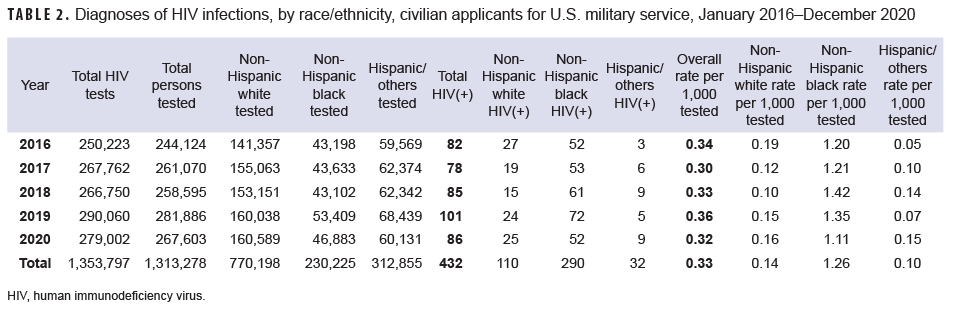
Throughout the surveillance period, annual HIV antibody seroprevalences among male applicants were consistently higher than among female applicants (Table 1, Figure 1). Seroprevalences were much higher among non-Hispanic Blacks, compared with other race/ethnicity groups (Table 2, Figure 2). During 2020, on average, 1 civilian applicant for service was detected with antibodies to HIV per 3,244 screening tests (Table 1).
U.S. Army
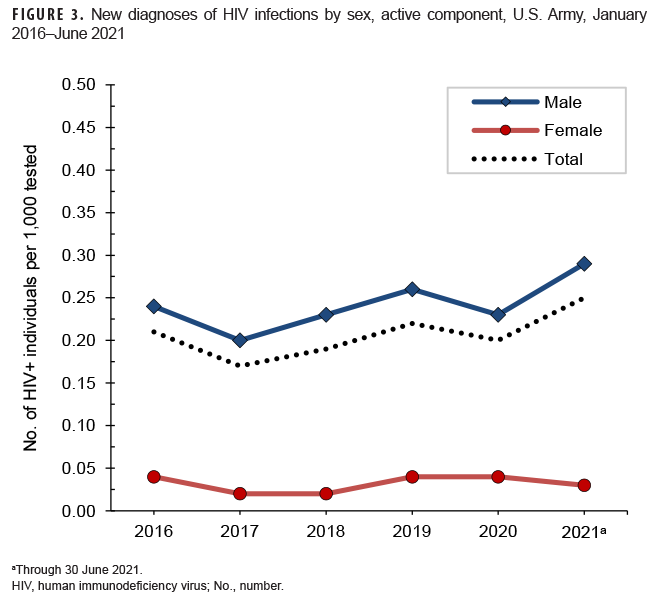
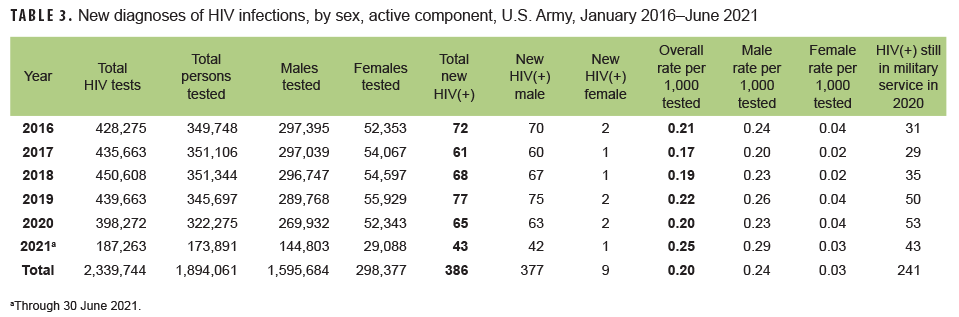
Active component: From Jan. 2020 through June 2021, a total of 496,166 soldiers in the active component of the U.S. Army were tested for antibodies to HIV, and 108 soldiers were identified as HIV antibody positive (seroprevalence: 0.22 per 1,000 soldiers tested) (Table 3). During the surveillance period, annual seroprevalences fluctuated between a low of 0.17 per 1,000 tested in 2017 and a high of 0.25 per 1,000 tested in 2021 (Table 3, Figure 3). Annual seroprevalences for male active component soldiers were considerably higher than those of female active component soldiers . During 2020, on average, 1 new HIV infection was detected among active component soldiers per 6,127 screening tests (Table 3). Of the 386 active component soldiers diagnosed with HIV infections since 2016, a total of 241 (62.4%) were still in military service in 2021.
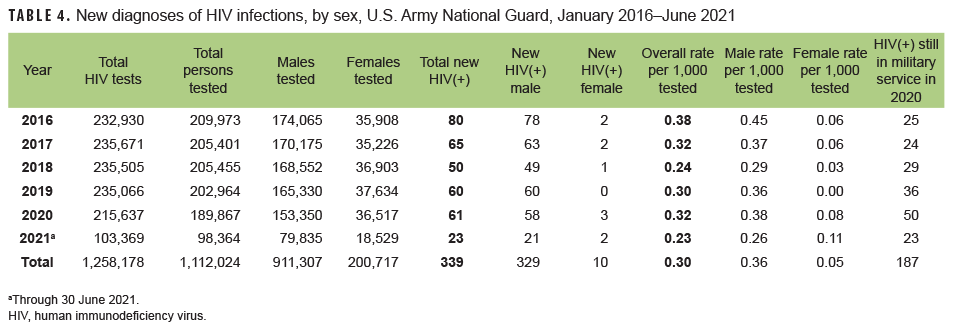
Army National Guard: From Jan. 2020 through June 2021, a total of 288,231 members of the U.S. Army National Guard were tested for antibodies to HIV, and 84 soldiers were identified as HIV antibody positive (seroprevalence: 0.29 per 1,000 soldiers tested) (Table 4). Among Army National Guard soldiers, annual seroprevalences decreased markedly from 2016 through 2018 (seroprevalences: 0.38 and 0.24 per 1,000 soldiers tested, respectively), increased in 2019 (0.30 per 1,000 tested) and 2020 (0.32 per 1,000 tested), and then decreased in the first 6 months of 2021 (0.23 per 1,000 tested). On average, during 2020, 1 new HIV infection was detected among Army National Guard soldiers per 3,535 screening tests. Of the 339 National Guard soldiers who tested positive for HIV since 2016, a total of 187 (55.2%) were still in military service in 2021.
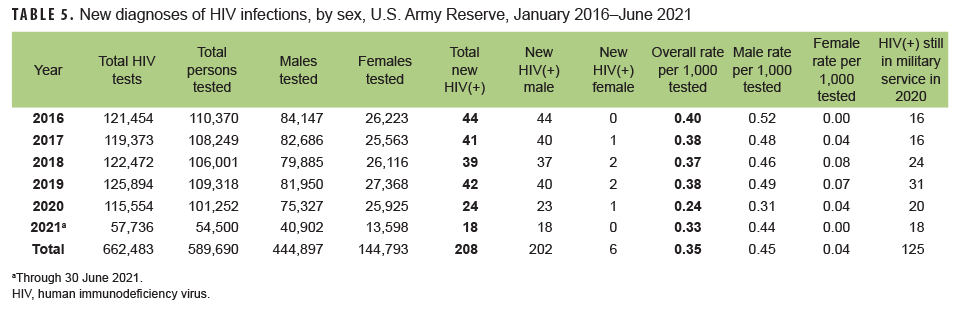
Army Reserve: From Jan. 2020 through June 2021, a total of 155,752 members of the U.S. Army Reserve were tested for antibodies to HIV, and 42 soldiers were identified as HIV antibody positive (seroprevalence: 0.27 per 1,000 soldiers tested) (Table 5). Among Army reservists during the surveillance period, seroprevalence was highest in 2016 at 0.40 per 1,000 tested, decreased slightly in 2017 to 0.38 per 1,000 tested, and then remained relatively stable through 2019. This pattern was followed by a considerable decrease in seroprevalence in 2020 (0.24 tested per 1,000), and an increase in seroprevalence in the first 6 months of 2021 (0.33 per 1,000). During 2020, on average, 1 new HIV infection was detected among Army reservists per 4,815 screening tests (Table 5). Of the 208 Army reservists diagnosed with HIV infections since 2016, a total of 125 (60.1%) were still in military service in 2021.
U.S. Navy
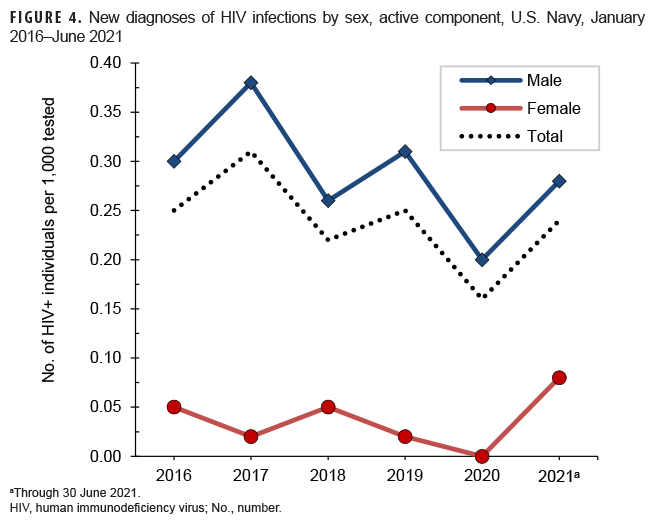
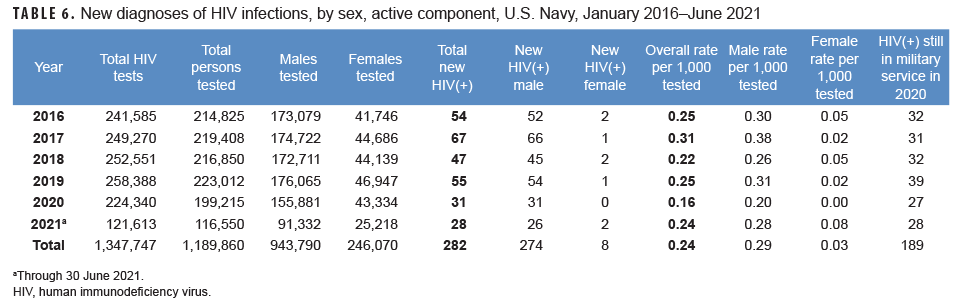
Active component: From Jan. 2020 through June 2021, a total of 315,765 active component members of the U.S. Navy were tested for antibodies to HIV, and 59 sailors were identified as HIV antibody positive (seroprevalence: 0.19 per 1,000 sailors tested) (Table 6). Among tested male active component sailors, full-year annual HIV antibody seroprevalences decreased 33.3% between 2016 and 2020 (Figure 4). Annual seroprevalences remained relatively low and stable among female sailors between 2016 and 2020, with an uptick in the first 6 months of 2021. However, during each year of the surveillance period, only 1 to 2 female sailors tested positive. During 2020, on average, 1 new HIV infection was detected among active component sailors per 7,237 screening tests (Table 6). Of the 282 active component sailors who tested positive for HIV since 2016, a total of 189 (67.0%) were still in military service in 2021.
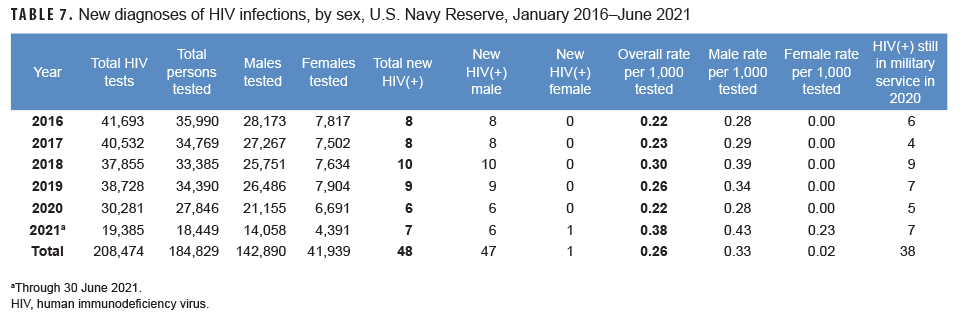
Navy Reserve: From Jan. 2020 through June 2021, a total of 46,295 members of the U.S. Navy Reserve were tested for antibodies to HIV, and 13 sailors were identified as HIV antibody positive (seroprevalence: 0.28 per 1,000 sailors tested) (Table 7). The HIV antibody seroprevalence among Navy reservists since 2016 peaked in the first 6 months of 2021 (seroprevalences: 0.38 per 1,000 sailors tested). Between 2008 and 2020, no female Navy reservist was detected with antibodies to HIV during routine testing (data not shown). However, 1 female Navy reservist tested positive in the first 6 months of 2021. On average, during 2020, 1 new HIV infection was detected among Navy reservists per 5,047 screening tests (Table 7). Of the 48 reserve component sailors diagnosed with HIV infections since 2016, a total of 38 (79.2%) were still in military service in 2021.
U.S. Marine Corps
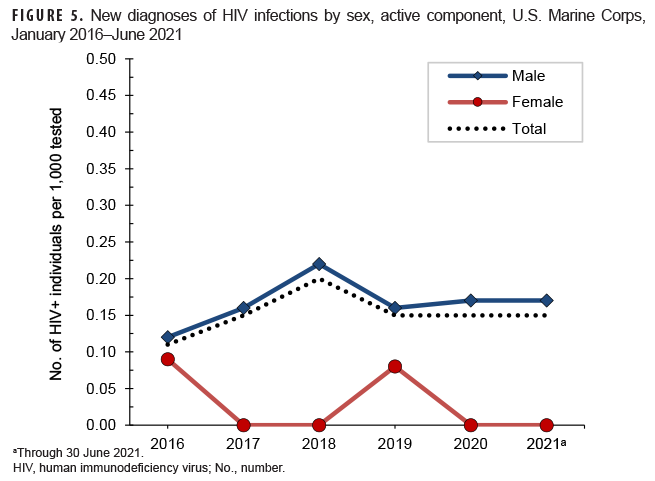
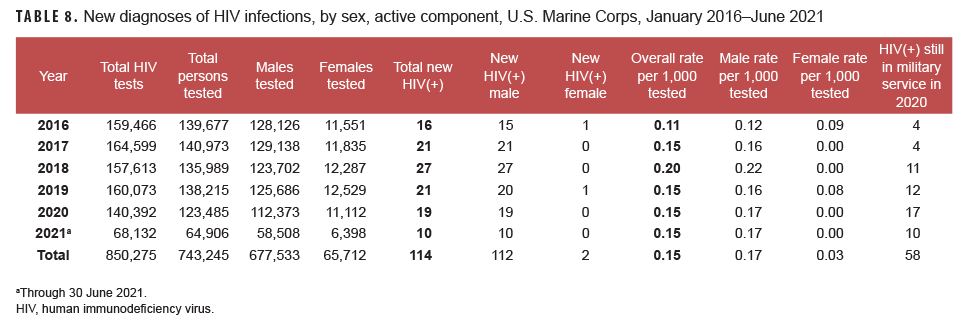
Active component: From Jan. 2020 through June 2021, a total of 188,391 members of the active component of the U.S. Marine Corps were tested for antibodies to HIV, and 29 Marines were identified as HIV antibody positive (seroprevalence: 0.15 per 1,000 Marines tested) (Table 8). From Jan. 2016 through June 2021, seroprevalences of antibodies to HIV remained relatively low and stable among routinely tested Marines (Figure 5). During 2020, on average, 1 new HIV infection was detected among active component Marines per 7,389 screening tests (Table 8). Of the 114 active component Marines diagnosed with HIV infections since 2016, a total of 58 (50.9%) were still in military service in 2021.
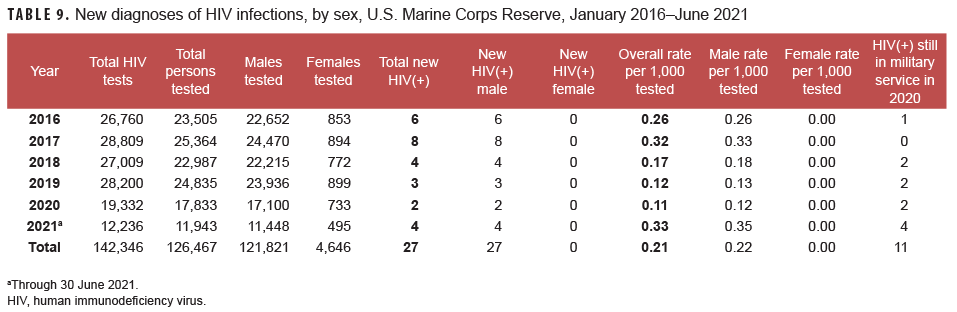
Marine Corps Reserve: From Jan. 2020 through June 2021, a total of 29,776 members of the U.S. Marine Corps Reserve were tested for antibodies to HIV, and 6 Marine Corps reservists were identified as HIV antibody positive (seroprevalence: 0.20 per 1,000 Marines tested) (Table 9). During the surveillance period, seroprevalences among Marine Corps reservists peaked at 0.33 per 1,000 tested in the first 6 months of 2021 and at 0.32 per 1,000 tested in 2017. Seroprevalence reached a low in 2020 at 0.11 per 1,000 tested. Of note, only 1 female Marine Corps reservist was detected with antibodies to HIV during routine screening in 2015; none were detected during 1990–2014 or during 2016–2021 (through June) (data not shown). During 2020, on average, 1 new HIV infection was detected among Marine Corps reservists per 9,666 screening tests (Table 9). Of the 27 Marine Corps reservists diagnosed with HIV infection since 2016, a total of 11 (40.7%) were still in military service in 2021.
U.S. Air Force
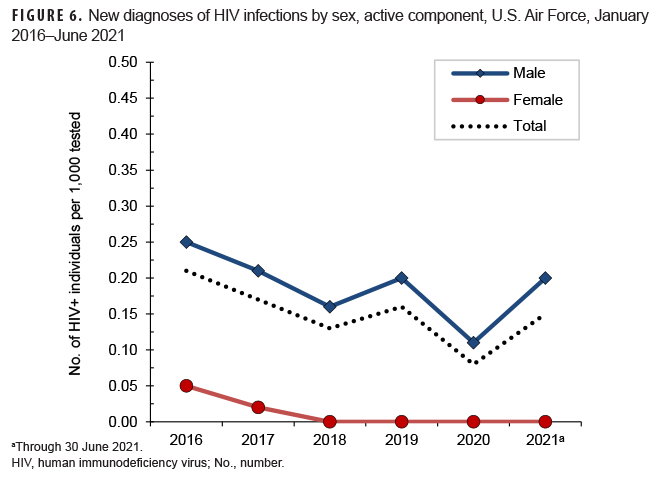
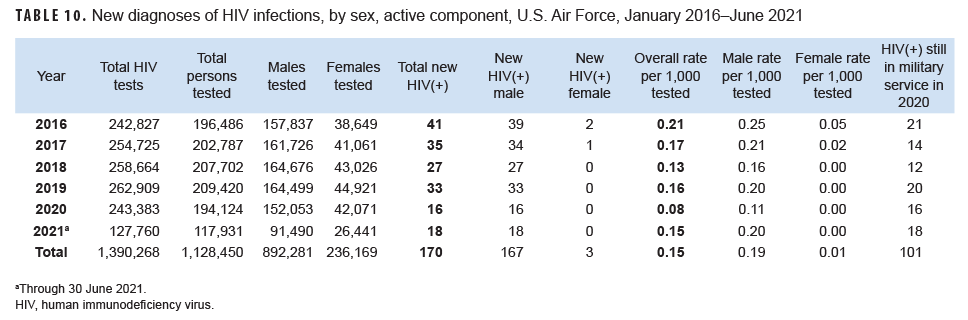
Active component: From Jan.2020 through June 2021, a total of 312,055 active component members of the U.S. Air Force were tested for antibodies to HIV, and 34 Air Force members were diagnosed with HIV infections (seroprevalence: 0.11 per 1,000 Air Force members tested) (Table 10). During the surveillance period, seroprevalences among male members ranged from a high of 0.25 per 1,000 tested in 2016 to a low of 0.11 per 1,000 tested in 2020 .(Figure 6). Among female Air Force members during the surveillance period, annual seroprevalences remained relatively low and stable. During 2020, on average, 1 new HIV infection was detected among active component Air Force members per 15,211 screening tests (Table 10). Of the 170 active component Air Force members diagnosed with HIV infections since 2016, 101 (59.4%) were still in military service in 2021.
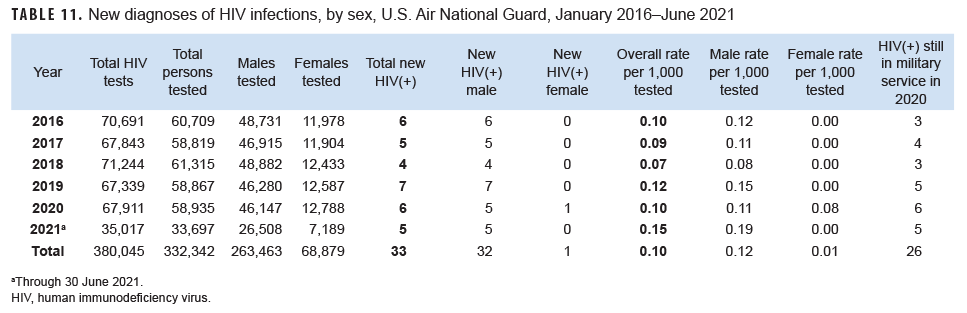
Air National Guard: From Jan. 2020 through June 2021, a total of 92,632 members of the Air National Guard were tested for antibodies to HIV, and 11 Air National Guard members were diagnosed with HIV infections (seroprevalence: 0.12 per 1,000 Air National Guard members tested) (Table 11). In 2020, 1 female Air National Guard member was detected with antibodies to HIV, the first since 2010 (data not shown). During 2020, on average, 1 new HIV infection was detected among Air National Guard members per 11,319 screening tests (Table 11). Of the 33 Air National Guard members diagnosed with HIV infections since 2016, 26 (78.8%) were still in military service in 2021.
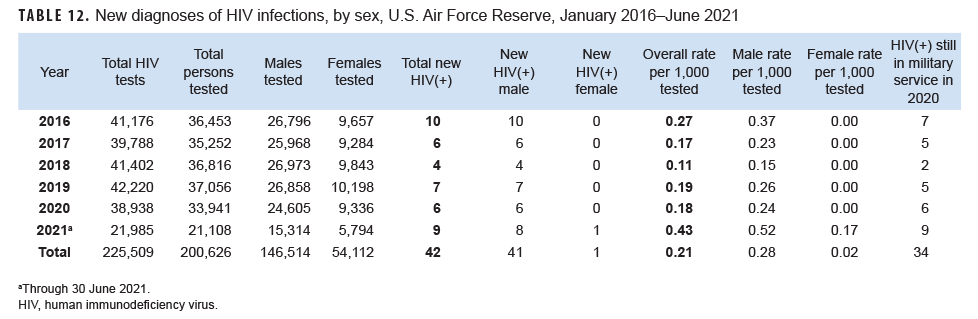
Air Force Reserve: From Jan. 2020 through June 2021, a total of 55,049 members of the Air Force Reserve were tested for antibodies to HIV, and 15 Air Force reservists were diagnosed with HIV infections (seroprevalence: 0.27 per 1,000 airmen tested) (Table 12). During 2020, on average, 1 new HIV infection was detected among Air Force reservists per 6,490 screening tests (Table 12). Of the 42 Air Force reservists diagnosed with HIV infections since 2016, 34 (81.0%) were still in military service in 2021.
Editorial Comment
The U.S. military has conducted routine screening for antibodies to HIV among all civilian applicants for service and all active and reserve component members of the services for more than 30 years.2,3,5,6 Results of U.S. military HIV antibody testing programs have been summarized in the MSMR for more than 2 decades.8
This report documents that, since 2016, full-year prevalences of HIV seropositivity among civilian applicants for military service have fluctuated between 0.30 per 1,000 tested in 2017 and 0.36 per 1,000 applicants tested in 2019. It is important to note that because applicants for military service are not randomly selected from the general population of U.S. young adults, seroprevalences among applicants are not directly indicative of HIV prevalences, infection rates, or trends in the U.S. civilian population. As such, relatively low prevalences of HIV among civilian applicants for military service do not necessarily indicate low prevalences or incidence rates of HIV among young adults in the U.S. in general.
This report also documents that full-year HIV antibody seroprevalences among members of the active components ranged from 0.08 per 1,000 tested (Air Force, 2020) to 0.31 per 1,000 tested (Navy, 2017). Full-year seroprevalences among the reserve/Guard components fluctuated between 0.07 per 1,000 tested (Air National Guard, 2018) and 0.40 per 1,000 tested (Army Reserve, 2016); the greatest variations in full-year seroprevalences were observed among Marine Corps reservists. During the surveillance period, full-year seroprevalences among applicants for service were highest in 2019 (0.36 per 1,000 tested) and then decreased in 2020 (0.32 per 1,000 tested). Full-year seroprevalence peaked in 2019 for active component service members of the Army, in 2017 for the Navy, 2018 for the Marine Corps, and 2016 for the Air Force. Among reserve and National Guard members, seroprevalence peaked in 2019 for the Air Force National Guard, 2016 for the Air Force reserve, in 2017 for the Marine Corps reserve, 2018 for the Navy reserve, and in 2016 for the Army National Guard and reserve.
Overall (Jan. 2016–June 2021) HIV antibody seroprevalences were highest among Army reservists, Army National Guard members, and Navy reservists and lowest among Air National Guard members, Marine Corps active component members, and Air Force active component members. Across active and reserve components of all services, seroprevalences continued to be higher among male than female service members.
There are several limitations that should be considered when interpreting the results of the current analysis. For example, because of the frequency of screening in the military (as an applicant, routinely every 2 years, and before and after overseas deployments), routine screening now detects relatively recently acquired HIV infections (i.e., infections acquired since the most recent negative test of each affected individual). As such, annual HIV-antibody seroprevalences during routine screening of military populations are reflective of, but are not direct unbiased estimates of, incidence rates and trends of acquisitions of HIV infections among military members.
In summary, the U.S. military has conducted comprehensive HIV prevention, education, counseling, and treatment programs for more than 30 years. Since the beginning of these programs, routine screening of all civilian applicants for service and routine periodic testing of all active and reserve component members of the services have been fundamental components of the military's HIV control and clinical management efforts.9 Summaries of results of screening programs such as those in this report provide insights into the current status and trends of HIV's impacts in various U.S. military populations.
References
- Centers for Disease Control and Prevention. Kaposi's sarcoma and Pneumocystis pneumonia among homosexual men—New York City and California. MMWR Morb Mortal Wkly Rep. 1981;30(25):305–308.
- Tramont EC, Burke DS. AIDS/HIV in the U.S. military. Vaccine. 1993;11(5):529–533.
- Brown AE, Brundage JF, Tomlinson JP, Burke DS. The U.S. Army HIV testing program: the first decade. Mil Med. 1996;161(2):117–122.
- Office of the Under Secretary of Defense for Personnel and Readiness. Department of Defense Instruction 6130.03, Medical Standards for Appointment, Enlistment, or Induction in the Military Services. 6 May 2018.
- Office of the Assistant Secretary of Defense. Health Affairs Policy Memorandum—Human Immunodeficiency Virus Interval Testing. HA Policy 04-007. 29 March 2004.
- Office of the Under Secretary of Defense for Personnel and Readiness. Department of Defense, Instruction 6485.01. Human Immunodeficiency Virus (HIV) in Military Service Members. 7 June 2013.
- Office of the Under Secretary of Defense for Personnel and Readiness. Department of Defense Instruction 1332.45, Retention Determinations for Non-Deployable Service Members. 30 July 2018.
- Army Medical Surveillance Activity. Supplement: HIV-1 in the Army. MSMR. 1995;1(3):12–15.
- Okulicz JF, Beckett CG, Blaylock JM, et al. Review of the U.S. military's human immunodeficiency virus program: a legacy of progress and a future of promise. MSMR. 2017;24(9):2–7.